In orthodontic treatment, archwire is one of the core components of the bracket correction system. If you are an orthodontist or a dental purchasing leader, this article will analyze the technical features, application scenarios and purchasing suggestions of orthodontic archwires from a professional perspective, helping you match your clinical needs more efficiently.
1. What Are Orthodontic Archwires?
Thin, flexible metal wires that are fastened to dental brackets are called orthodontic archwires. Over time, these wires gradually shift the teeth into the proper position by applying light, continuous pressure. These wires are known as “arch wires,” and the lower arch is formed by the wires on the lower teeth, while the upper arch is formed by the wires on the upper teeth.
They act as a guiding engine for the teeth and are essential for controlling tooth movement. Without it, your crooked teeth would never move. These braces wires come in different sizes and have different material compositions.
2. What Is The Function of The Archwires?
As a dynamic mechanical component of the orthodontic system, the orthodontic archwires achieves passive movement of teeth through an accurate compression mechanism. During the initial treatment stage, orthodontiologists select nickel-titanium alloy archwires with appropriate elastic modulus. Their shape memory properties can apply a continuous orthodontic force of 0.5 to 1.5N/cm² to the misaligned dentition. This mechanical stimulation triggers alveolar bone remodeling by activating the proliferation of osteoclasts on the pressure side and osteoblasts on the tension side, achieving a monthly displacement of 0.1 to 1mm for the teeth.
Archwires perform three essential functions:
| Vector Guidance | Establishing ideal dental arch curvature through preformed wire shaping |
| Force Delivery | Translating bracket system constraints into directional tooth movement |
| 3D Control | Adjusting axial inclination and rotational positioning via torque engineering |
The dynamic adjustment mechanism runs through the entire treatment cycle: follow-up is conducted every 4 to 6 weeks, and orthodontists maintain the optimal orthodontic force of 20 to 150g/cm by replacing the archwire. In the middle and later stages of treatment, it transitions to the stainless steel archwire stage (0.016×0.022 inches to 0.019×0.025 inches), with an elastic modulus of 210GPa. This enables the establishment of an accurate three-dimensional mechanical system, allowing for fine regulation of root tip movement and occlusion.
Profit’s three-stage theory (Profit, Fields, & Sarver, 2018) is followed by this biomechanical system: initial alignment → vertical control → torque fine-tuning, which leads to 80–90% repositioning of the dental arch and functional occlusal reconstruction. According to clinical data, the archwire system’s standardized application can maintain the root resorption rate below the safe threshold (< 2mm) and boost orthodontic treatment efficiency by 40%.
3. The Science Behind Orthodontic Archwires
Today’s archwire is an engineering marvel, in contrast to orthodontics’ homogeneous approach in the early 20th century. Materials science holds the key to their success: the right alloy selection has a direct impact on treatment speed, comfort, and result.
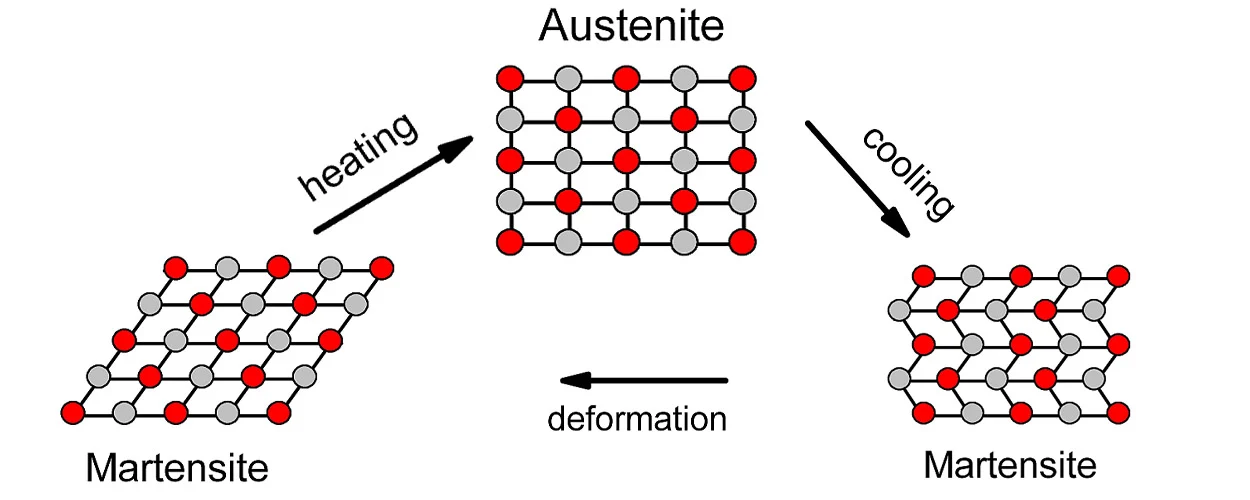
Consider NiTi (nickel-titanium) wire. Almost no one anticipated that NiTi would have dental potential when Dr. William J. Buehler first noticed its “shape memory” qualities in the Naval Research Laboratory in the 1960s. These days, this alloy is a major solution to the issue of crowded teeth because it can “remember” the patient’s ideal dental arch shape and can withstand up to 8% strain (whereas steel can only withstand 1%).
4. Classification of Orthodontic Archwires
Orthodontic archwires can be classified into three major types based on the different material properties:
A. Nickel-Titanium Archwires (NiTi)

B. Stainless Steel Archwire

C. Beta-Titanium Archwire

5. Clinical Selection Criteria for Orthodontic Archwires
Match elasticity to strength according to the treatment stage
For initial correction, superelastic nickel-titanium archwires should be given priority to reduce patient discomfort. In the middle and later stages, stainless steel or β -titanium bow wires are replaced to precisely control the force.
Focus on the surface treatment process
High-quality bow wires should have a smooth surface (such as electrochemical polishing) to reduce the friction of the brackets and avoid mucosal irritation.
Standardized dimensions and memory performance
Select archwires that meet the AAO (American Orthodontic Association) standards to ensure compatibility with mainstream bracket systems and high shape memory stability.
6. Clinical Usage and Maintenance Suggestions
- The archwire replacement cycle: The patient’s tooth movement speed and the level of orthodontic archwires fatigue determine how often it is adjusted, which is typically every 6 to 8 weeks.
- Advice for patients: Keep in mind to refrain from chewing hard objects, apply orthodontic wax to ease any initial discomfort caused by friction, and clean the archwire on a regular basis to avoid plaque buildup.
- Storage requirements: To prevent oxidation or deformation, unopened bow wires should be kept in a dry atmosphere.
7. Why Choose Our Orthodontic Archwires?
As an exporter specializing in the research and development of dental consumables for 15 years, we offer:
Strict quality control: products are ISO 13485 certified, FDA/CE compliant and batch traceable.
Diversified choices: covering the full range of sizes from 0.012″ to 0.021×0.025″, supporting multi-material customization such as nickel-titanium, stainless steel, beta-titanium and so on.
Case Sharing: Bow Wire Solution to Enhance Clinic Efficiency.

A chain of dental clinics in Barcelona, Spain, reduced the average treatment cycle of initial cases by 15% and the time for follow-up adjustments by 20% by using our Nitinol archwires. The doctor’s feedback is that “the shape memory stability of the archwire significantly reduces the complexity of the operation, which is especially suitable for teenage patients.”
Conclusion
Despite their small size, orthodontic archwires are essential components that influence the correction effect. Selecting the appropriate archwire can boost patients’ confidence in the course of treatment in addition to increasing the effectiveness of diagnosis and treatment. Please do not hesitate to contact us at any time if you would like free samples or more information about our products.
References
- Shah, S. J., Ali, M., & Matthews, M. E. (2015). Orthodontic materials and techniques. Journal of Clinical Orthodontics, 49(8), 23-34.
- Ribeiro, T. K. S. J., Silva, S. A. S., & da Silva, D. P. (2020). Biological mechanisms of tooth movement: A review. European Journal of Orthodontics, 42(2), 55-64.
- Proffit, W. R., Fields, H. W., & Sarver, D. M. (2018). Contemporary orthodontics (6th ed.). Elsevier.